The United States has some of the highest maternal mortality rates in the developed world — and unlike most other first-world countries, our rates are going in the wrong direction.
American women are three times more likely to die during or after birth than women in Great Britain and eight times more likely than women in Scandinavian countries.
But despite the prevalence of major risk factors such as low access to prenatal care, a high poverty rate and a largely rural population, West Virginia, is bucking the maternal mortality trend. Maternal deaths are not only low, they’re also stable.
Part of that may be due to statewide initiatives to improve outcomes.
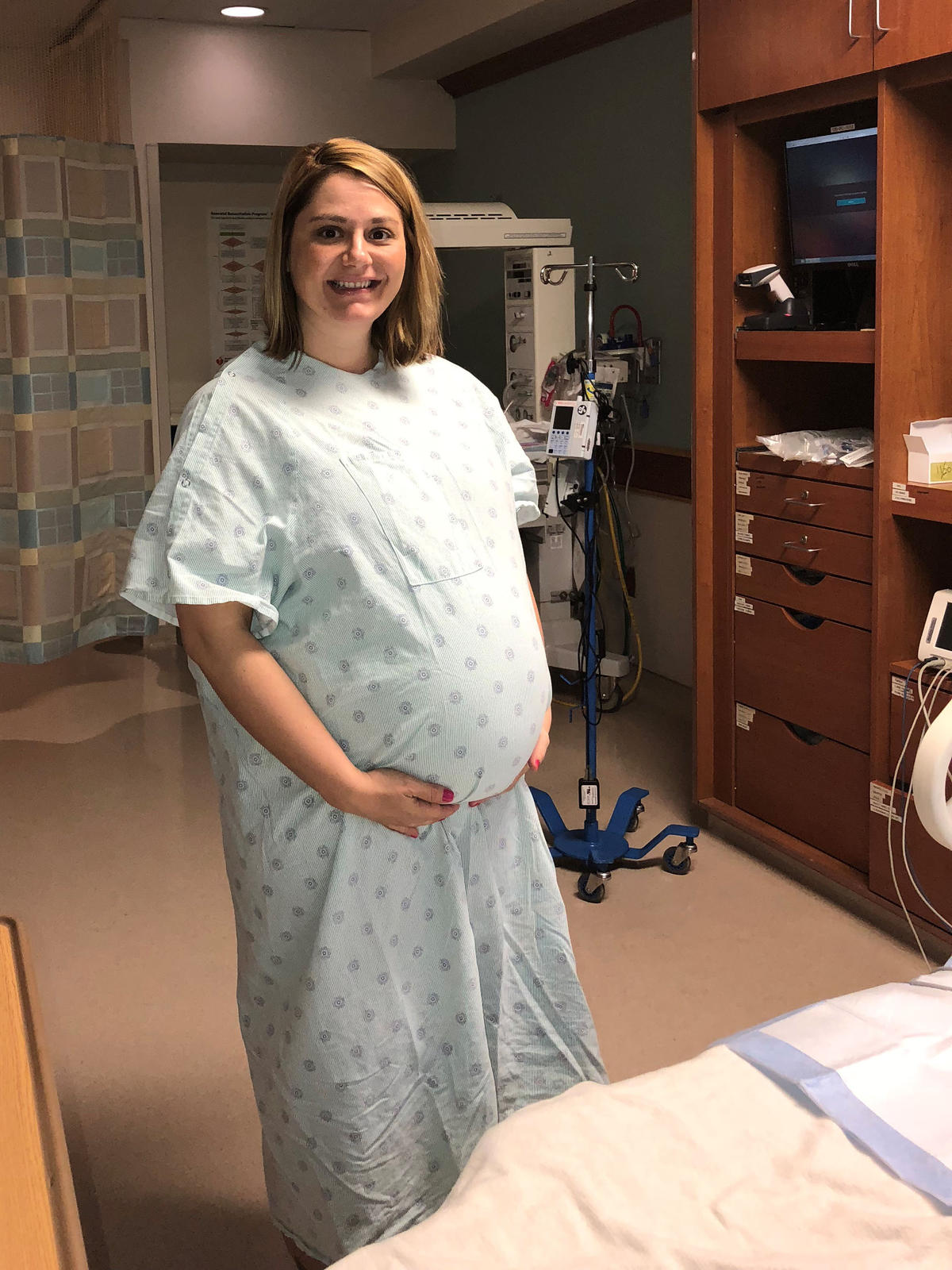
Lauren Headley
When Lauren Headley was 35, she got pregnant. Her age categorizes her as high-risk, but she is a nonsmoker and was a Zumba teacher at a healthy weight at the time she conceived.
About six months into her pregnancy, though, Headley was diagnosed with gestational diabetes. Her obstetrician was concerned that, as a result, her baby would be born large and wouldn’t fit through her birth canal. So at around 39 weeks, doctors induced labor. The baby girl was born healthy and neither mother or infant had any complications.
Then on the 10th day after she gave birth, Headley woke up bleeding.
“But this was like gushing and red clots of Jell-O,” she said.
She called her doctor’s office and her doctor told her that some bleeding was normal but, if it continued, to go to the emergency department or to call back. So she got into the shower to see if that would calm things down.
“As I’m in the shower, the blood just pours out,” she said. “I mean cups of red Jell-O is what it looks like and it’s just pouring out. And I get really weak and I sit down in the shower and yell for my husband, and he comes in and he looks in there and he’s like ‘Oh dear God, you need to call your doctor back. There’s no way this is normal.’”
Headley was taken by ambulance to the emergency department at Thomas Health, where she was diagnosed with a severe postpartum hemorrhage — which is one of the leading complications that causes maternal mortality in the United States.
Postpartum hemorrhage 10 days after birth is admittedly pretty rare, but how well a hospital is prepared to deal with obstetric emergencies can mean the difference between life and death for someone like Headley.
Which may be part of why West Virginia’s rates are so low.
West Virginia’s rates are low — but why?
West Virginia actually ranks 5th in the country — tied with Hawaii — for least number of maternal mortality deaths in the nation — behind California, Massachusetts, Colorado and Nevada, according to data from the Centers for Disease Control and Prevention.

Maternal deaths in West Virginia related to pregnancy and childbirth have bounced between one to four deaths a year during the past 11 years. Even though West Virginia is a small state and has few births annually, this is a pretty low rate and surprising because West Virginia is poor, rural and has higher rates of comorbidities, which are all risk factors.
But when you try to dig into the numbers, “it’s hard to know exactly why our rates are lower,” said Amy Tolliver, director of the West Virginia Perinatal Partnership. She said over the last 10 years, they’ve been working closely with all of the hospitals in the state that deliver babies to improve the care they offer to moms.
“We have been implementing different training programs specifically around maternal hemorrhage — that is one of the bigger drivers that we see in regard to maternal morbidity and nationally in terms of maternal mortality,” Tolliver said.
Tolliver said every hospital in the state that delivers babies has a specific set of protocols they are supposed to adhere to in the event of complications like uncontrolled postpartum bleeding.
“To have the crash carts available with all of the equipment necessary, to have trainings in place, and to continue doing those staff trainings — we think that’s one of the biggest factors in improving care is practicing for the high-risk patient.”
“I think we also do a good job in this state of accepting the fact that we have a lot of the risk factors that increase the risk for maternal mortality,” said Dr. Ally Roy, an obstetrician at Marshall Health.
Roy delivers babies at Cabell Huntington Hospital. When a patient is admitted there, she says there is a checklist the staff goes through with the patient. If they meet the criteria for moderate or high risk for postpartum hemorrhage, they receive intervention at delivery time aimed at reducing their risk. Anecdotally, she said, the protocols have greatly improved outcomes for patients with postpartum hemorrhage.
“When you have an emergency, you want people to be able to react smoothly and seamlessly,” said Tolliver. “There should be no downtime in trying to figure out what they need to do next. It needs to be very quick, very regimented, getting the process in place.”
In an email exchange with Thomas Health, the hospital Headley was taken to, a representative said that Thomas has protocols in place for how to deal with hemorrhages that were developed in conjunction with the statewide initiatives.
But experts working in this field in West Virginia say there’s still work to be done.
In 2008, West Virginia established a maternal mortality review committee made up of experts from across the state that basically looks at all of the data around deaths linked to pregnancy and childbirth and sees what happened. They then make recommendations based on the findings. About half of U.S. states currently have such committees.
“One of the first things that we did find was that some of our women who were postpartum may have presented in an emergency room with a severe headache and other symptoms, but they weren’t caught quickly enough in regard to understanding that that was preeclampsia, for example, that they may have been experiencing,” said Tolliver. “So there were some efforts put together to do some education with our emergency room staffing.”
Preeclampsia is a pregnancy complication that is usually characterized by high blood pressure and, if untreated, can cause organ damage and even death.
Last year, the committee recommended a renewal of those education efforts, so the Perinatal Partnership is getting ready to go out around the state to do more trainings.
Tolliver said the objective is to have caregivers “be prepared to be looking at the patient just a little bit differently [and] to ask the question, ‘Has she given birth recently?’ Those answers to those questions may drive the care in a different direction and get to the bottom of what is going on with her much more quickly,” she said.
So is there anything women could do to protect themselves against dying in childbirth? First, say experts, understand that women can experience life-threatening complications during childbirth, thus they recommend that women listen to their bodies, advocate for themselves, and talk about risk with their care team.
This article was originally published by West Virginia Public Broadcasting.
Appalachia Health News is a project of West Virginia Public Broadcasting, with support from Marshall Health and Charleston Area Medical Center.