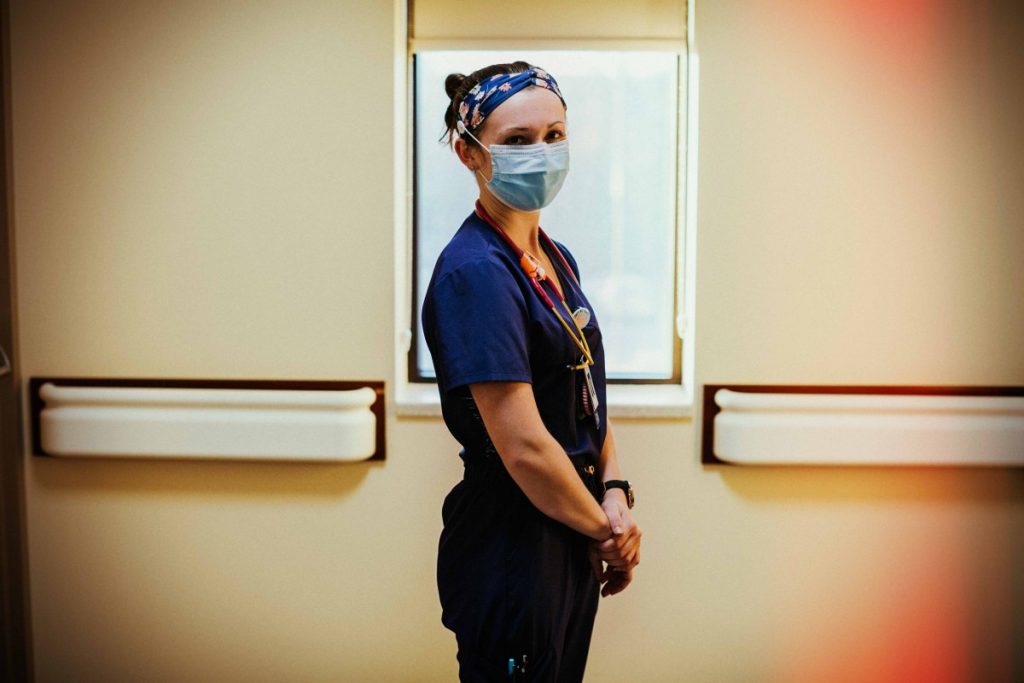
Chelsea Jacobs is a courageous woman, a nurse who brings bravery into the hospital – the hard-earned kind you get when you spend your weekends barrel horse racing.
She’s been on the job at the Berkeley Medical Center in Martinsburg, West Virginia, for the past three years. Like many nurses, Chelsea inspires confidence with her mixture of clinical competence and compassion. Her bright eyes peek out between her headband and face mask, ready for whatever may happen.
“It came fast,” she says of the COVID-19 pandemic. “We heard about it and then – about two weeks later, boom, it was here. None of us had any chance to grasp it until it was already here. We felt like we were chasing our tails and trying to catch up.”
“We did not know what we were treating,” Chelsea remembers of those early days, amazingly now a year behind her. “We went into it thinking this is a bad virus and we see people on TV dying. At first, there was not enough personal protective equipment (PPE) for us. That part was scary. I mean, what am I risking taking home to my family?”
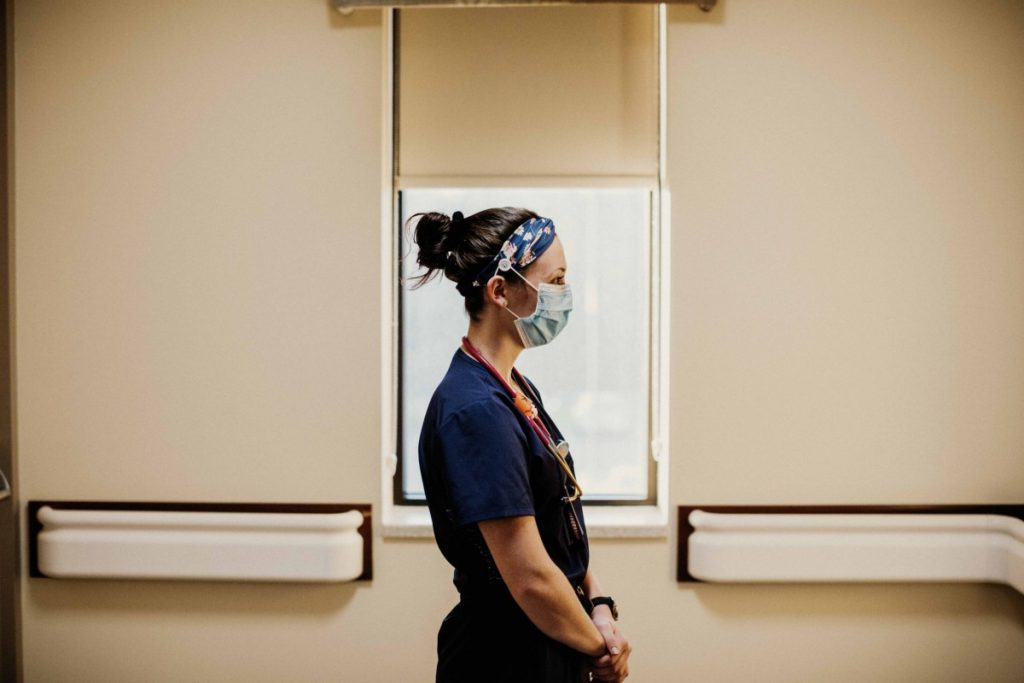
During dark pandemic days, Chelsea takes care of sick patients inside a scary, lonely hospital. She processes her fears as she completes her daily tasks – passing medicines, coordinating surgeries, counseling patients. There are no days at home to get organized and up to speed on COVID.
Chelsea says the pandemic is an ever-evolving event, where the stresses change over time. As soon as you master one aspect, “Stuff changes every day,” she says. With COVID testing finally sorted out and PPE available, other problems arise. The pandemic is an extra-thick layer of problems piled on top of the usual demands of patient care inside the hospital.

When the pandemic shutters the hospital’s doors to visitors, Chelsea says everything gets exponentially harder. “There is a communication barrier with patients. They are told they have this horrible virus and then their family can’t be with them in the hospital,” she says. “It’s a terrible situation.”
It’s not just the patients who suffer when the hospital access is restricted. Nurses also find themselves isolated and stressed. Chelsea says she’s dealt with the difficult decision of when to call a dying patient’s family, knowing they couldn’t come to the bedside and say goodbye. “It was very stressful as a nurse. I hated that part of it. I can still remember the day. It was an awful experience.”
But her support system, Chelsea says, is what’s helped her through these painful moments. Her partner works in healthcare as well and the teamwork with her coworkers has been a bright spot.
“I am working on a COVID unit and we have a diversity of nurses from all over the hospital. OR (operating room), medical-surgical, ICU, nurses from different backgrounds. There is always someone to learn from. That part has been good.”
But the past year has been exhausting, Chelsea says. The one thing that could help in the short term: “Get me some N95’s that are comfortable,” she says without hesitation. This piece of equipment, critical to safely working during a pandemic, could use some major improvement in the comfort department – at least for one nurse working a 12-hour shift.
Healthcare is Human is an independent podcast produced by Ryan McCarthy, Shruthi Sreekumar, Molly Humphreys and Kym Mattioli out of Martinsburg, West Virginia. Listen to their latest episodes on their Soundcloud or keep up with their latest work on Facebook.