You can still find West Virginians sporting WW2 and Korean War vet hats, wars that were fought more than 70 years ago, as well as hats representing Vietnam, the Gulf War, Iraq and Afghanistan. More than 145,000, or nearly 10 percent, of the state’s population have served their country.
Over the course of their service, many were exposed to everything from heavy smoke, to oil fires, to the highly-toxic chemical Agent Orange. This means many vets are either elderly or they have preexisting conditions, making the veteran population particularly susceptible to the new coronavirus.
“Agent Orange has been associated with certain cancers, like Hodgkin’s disease, lymphomas, lung and upper respiratory cancers and also Parkinson’s disease [and] diabetes,” said Dr. Prasad Devabhaktuni, a pulmonologist and the head of the emergency department at the Louis A. Johnson VA Medical Center in Clarksburg. “If the individual has associated burn pit lung injury or problems like hyperreactive airways or asthma, then we would consider they are at increased risk for complications. Complications, pneumonia or respiratory failure, things like that.”
George Smith normally works as a clerk, but on this day he’s screening visitors at the temporary carport erected at the hospital’s entrance. Smith asks the visitor if they’ve been in high-risk coronavirus areas, met someone who has the coronavirus or if they are feeling sick. If they don’t, he gives them a green armband to wear while they’re on the hospital grounds.
Helping Smith work the carport are a VA dentist and her assistant. It’s an unlikely team, but since President Donald Trump declared a state of national emergency, the VA has reorganized resources to address the crisis, including assigning people to where there is need.
Right now, the need is at the hospital entrance. Staff has been trained to safely screen patients and visitors for the coronavirus, according to Dr. Glenn Snider, the director of the facility.
“Training on things such as how to apply and utilize a protective mask, how to utilize an N95 mask, how to use portable ventilator equipment that are used, that is used to protect staff from airborne droplets and viruses,” he said.
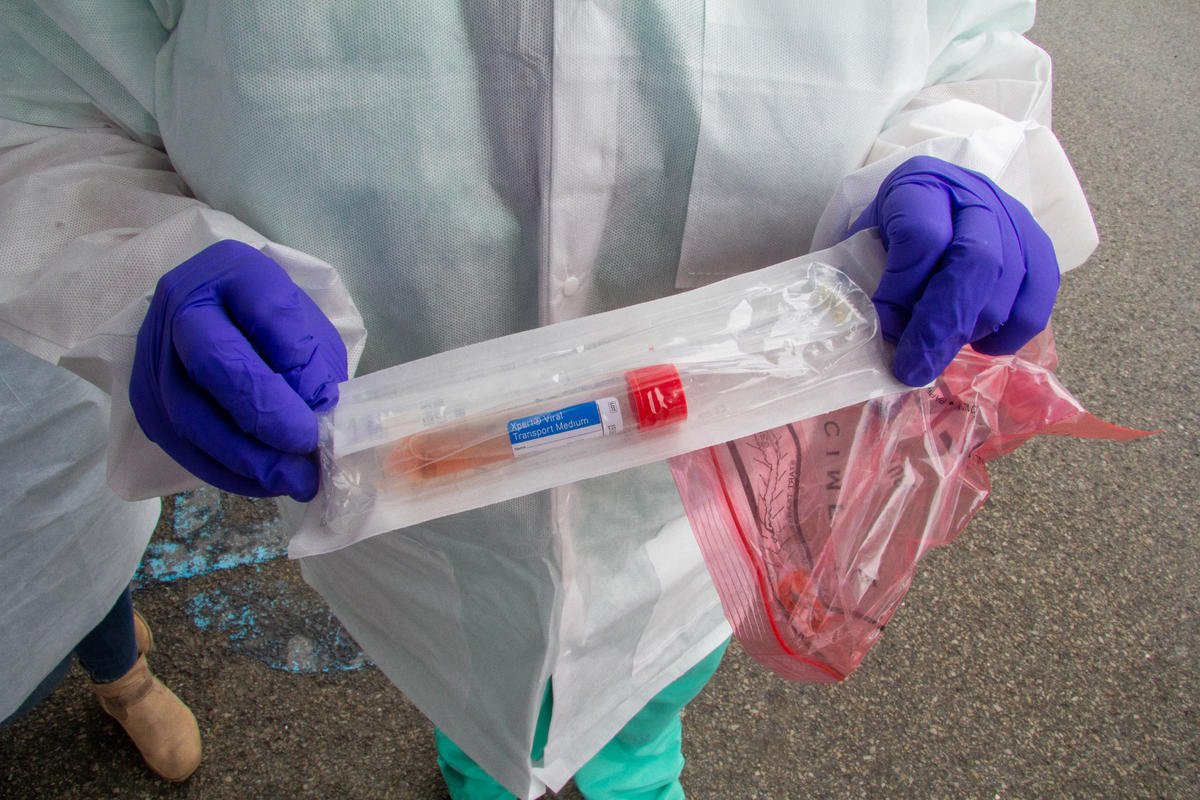
Behind Smith’s temporary carport is a tent where staff are also screened. If the staff or visitor replies “yes” to any of Smith’s questions, they are directed to an area where two registered nurses are garbed in full protective gear — with gowns and portable ventilators — that look like bicycle helmets with face masks and tubing. The nurses are armed with thermometers and coronavirus test kits, which allows them to check temperatures and swab for the virus.
“If the individual is minimally symptomatic, they’re sent home with instructions on how to manage themselves at home,” Snider said. “They’re also given phone numbers to call in to speak to staff if they have an acceleration of symptoms or if they have other questions.”
An acceleration of symptoms means shortness of breath, or persistent pain or pressure in the chest. Snider said if you do plan to come to the hospital, please call beforehand so they can be ready for your arrival.
“Our goal being, ‘Let’s reduce exposure to as many veterans and as many staff as is possible,'” he added. “But of course, if the individual is in respiratory distress, then the best course of action is to present to the emergency department immediately and for many veterans that means calling 911 for medical transportation.”
In the front lobby of the hospital, there is a newly constructed negative air pressure hallway that is made up of walls made from plastic sheeting, wooden wall joists and duct tape sealing the plastic to the floor. When the hospital gets a coronavirus patient, they’ll go from outside straight into this special hallway, avoiding the lobby. Here, the air is sucked in, and can’t pass out, protecting other patients and staff from potential exposure to the coronavirus.
In the emergency room, which is normally packed, but there aren’t any patients. Although the hospital is open, staff said veterans are apparently staying home in accordance with the governor’s stay at home order.
While the VA focuses mostly on veterans, in 1982, Congress passed a law mandating that the agency provide backup healthcare services to the country in times of crises. Dr. Snider said if the VA was ordered to it would help the general public.
“At this time, I don’t believe that has been invoked, but if it were to be invoked, the medical center is aware of that mission of the VA and we would do everything we could to work with community partners in serving not only veterans, but those in our community,” he said.
And while current cases in West Virginia remain relatively low, if hospitals were to see an increase in veteran patients, then Snider said the VA currently has everything they need to care for vets.
“Based on the calculations we’ve been given from central office, we should be able to handle any projected surge that were to occur, but as a reminder, sometimes we can’t predict the behavior of some viruses in some populations,” he said. “So, I can’t guarantee 100 percent, but I can tell you that today we have everything that we need to care for our patients.”
In the meantime, the Clarksburg VA hospital is tracking everything from lab materials, to protective equipment, to hand sanitizer, to ventilators to ensure that if it’s needed, they’ll be ready.
If you’re a veteran located in north-central West Virginia, you can reach the Clarksburg VA at 304-623-3461, extension 3450. For veterans in other parts of the state that are experiencing symptoms, call your local VA hospital or outpatient clinic.
This article was originally published by West Virginia Public Broadcasting.