Part 1: Why W.Va.’s Largest Needle Exchange Closed
In December 2015, with support from the city of Charleston, the Kanawha-Charleston Health Department launched a harm-reduction program that included a needle exchange. The primary goal was to reduce the risk of diseases commonly spread by sharing needles.
Now, only thing that remains of the harm reduction program is a syringe kiosk where people can deposit used hypodermic needles.
At its peak the program served more than 400 people a week,mostly from Kanawha County. But some came from surrounding counties as well,a factor that became a point of contention for many in the city.
“It became basically, a line of people just to line up to get needles between 10 and 4 on any given Wednesday,” said outgoing Charleston mayor, Danny Jones who been an outspoken critic of the program.
In the months before it closed, Jones publicly called the program a “needle mill” and “mini-mall for junkies.”
“On any given Wednesday, they might have given out 12,000 needles,” he said during a recent interview.
In reality, the average number of needles given out during the weekly Wednesday exchange was about 5,000 serving about 190 visitors, according to data obtained from the health department. That’s about 26 needles per person, per week. The highest number of needles the program ever gave out in a single week was just over 11,000 to 417 people.
While 5,000 seem like a lot, the average heroin user injects several times a day. So 26 needles a week gets a person about three injections a day with a clean needle.
“A syringe exchange program should really be called a harm reduction program,” said Dr. Artis Hoven, an infectious disease specialist with the Kentucky Department of Health.
She said harm reduction is an all-encompassing idea to reduce the risk of many things associated with addiction such as “provide naloxone, provide referral to care for people with substance use disorder, they do HIV and Hepatitis C testing.”
And in Charleston, it seemed to work.
While the Charleston program was open, the city did not see an HIV outbreak, according to interviews conducted by Charleston-Gazette Mail. During that same time period, 15 counties in southern West Virginia did have a small HIV outbreak — none of the three counties where the outbreak started had a harm reduction program, according to a Centers for Disease Control and Prevention Report.
Recorded incidents of Hepatitis C rates in West Virginia did increase — by a lot — during the course of the program, but so did efforts to test more people.
But in Charleston, reports of discarded needles in the community began to skyrocket and people were alarmed.
Firefighters reported having to crawl over them while putting out fires in abandoned structures; a local elementary school requested a biohazard container from the city so they could clean up an alley before school; and police officers reported finding huge numbers of syringes on people who were arrested.
Both the Fraternal Order of Police and the Charleston Professional Firefighters Association wrote letters to City Council expressing major safety concerns for first responders.
Concerns might have been exacerbated because the program grew really fast. In the two years the program was open, more than 651,000 needles were distributed. Only about 66 percent of those needles were returned.
According to the Centers for Disease Control and Prevention, the risk of contracting HIV is nominal for for healthcare professionals stuck by needles on the job — around .3 percent — with some studies suggesting even less. Outside experts like Peter Davidson from the University of California San Diego say needle litter is an annoyance but not the major public health concern an HIV or Hepatitis C outbreak would be.
“No one in the world has ever obtained HIV from stepping on a needle in the street,” said Davidson. “Needles in the street are a piece of trash. It’s not something you want seeing laying in the gutter, but they’re not actually a very hazardous object.”
In some ways, it doesn’t matter what the risk is. If someone finds a dirty needle on a playground or in a shopping mall bathroom, public reaction is strong. And for non-users, any risk of contracting HIV or hepatitis from a dirty needle is too much.
But closing a harm reduction program in the biggest city in the state could have huge public health implications for the region, according to former state Commissioner for Public Health Rahul Gupta. Gupta said it’s “not in the best interest of the community” when needle exchange programs like this one are shut down “reactively.”
“It plays into that stigma and is more harmful long-term than it is beneficial,” he said in an interview shortly before he left his job.
Gupta said it’s more harmful because not only are you removing your best tool for preventing needle-born illnesses, but, as we’ll hear later in this series, the closure may impact public perception and support for other harm reduction programs across the state that are trying to open or stay open.
Part 2: Public Safety and Public Health
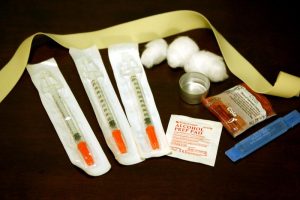
Best practices for harm reduction programs call for flooding a community with clean hypodermic syringes. Research shows that in addition to reducing the prevalence of blood-borne pathogens in the community, well-run programs help remove potentially infectious syringes from the community. But some people say that wasn’t happening in Charleston.
Mayor Danny Jones said the city tried numerous times to complain and the Kanawha-Charleston Health Department didn’t do anything to address their concerns.
Then city health officer Michael Brumage took issue with that accusation,pointing to efforts, such as the founding of the statewide harm reduction coalition. He said one of the objectives of the coalition was to bring needles into other communities so there wouldn’t be such a burden on the city.
But in October 2017, the city public safety office established a code for needle pickup calls to help the city accurately collect data on locations, numbers and types of needles to be picked up.
About a week later, the city proposed running a pilot program with retractable needles. The idea was that if the needles could only be used once and then retract into a plastic chamber, it would reduce the risk of needlestick injuries to the community and first responders.
At the time, Brumage was all for the idea. He wrote an an email, which was part of documents released to West Virginia Public Broadcasting through a Freedom of Information Act request, to city attorney Paul Ellis.
“[T]he limitations … are acceptability and cost. Should we get support or donated supplies, I am all in for a pilot with evaluation. This could be a very interesting trial. We would like to bring in some researchers for this as well. Let’s do it! It’s worth a shot.”
Over the next few weeks, the Charleston Fire Department found a manufacturer willing to donate the needles in exchange for tracking how well they worked. After consulting with Brumage and his staff, the city requested 250,000 needles from the manufacturer for a six-month trial.
Everything seemed to be on track to start a pilot project using retractable needles in early spring 2018.
At least that’s what the city thought. Meanwhile, Brumage was in communication with a researcher at Johns Hopkins University in Baltimore, Maryland. The researcher reinforced something with him that he said he already knew — that “retractables were unpopular among people who used IV drugs.”
In 2010, the national Harm Reduction Coalition issued a statement against auto disable syringes. They said the syringes do little to help control epidemics of HIV, hepatitis C, and other blood-borne viruses among people who inject drugs because many people inject drugs a half dozen times a day. Without needles you can use more than once, users revert back to sharing equipment.
“So, at that point I was kind of in a bind since I told the city we would implement the retractable syringe program. But now knew if I did, we’d actually be putting the public at risk,” said Brumage.
So given the current recommended practices, Brumage and the Johns Hopkins researcher decided to reduce the pilot instead to about 10 to 12 people. In meeting minutes from a call, also released in the FOIA,, Brumage’s staff appeared to confirm the new plan with the company that had agreed to donate the syringes.
Brumage said he thought the needle manufacturer then told the city about the change. But no one did. So city officials said they felt blindsided several weeks later when they learned the pilot program no longer included the entire patient population.
“They refused retractable needles,” Jones said in an interview.
It was more complicated than that, but it probably felt like a refusal to the city because of the change in plan wasn’t communicated. And I mean, remember, law enforcement, emergency responders and some members of the community were now expressing a lot of concern about needle litter and felt like they had to do something.
“I want to protect the public. I want to protect the law abiding public,” said Jones.
In late March of this year, Charleston Police Chief Steve Cooper decided — as he was legally empowered to do — that the health department may only give out retractable needles.
Essentially, Brumage said, the police were “ directing the health department to adopt — what appeared to be from the medical literature to be dangerous and unethical practices.”
But other public health experts said making a harm reduction program fit the needs of the community takes a lot of compromise.
“Public health has never been and will never be about my way or your way. It will always be what’s the best way to input science and marry it with art and put it into practice,” said former public health commissioner Rahul Gupta.
From a public health perspective, harm reduction programs are still the best tool the city a city? has to prevent the spread of needle born illnesses. But politically — at least in the state’s largest city — it’s closed indefinitely.
Part 3: Community Acceptance, Perception and Stigma

Less than two years after it began, the Kanawha-Charleston Health Department shut down it’s harm reduction program. Among other things, the program provided thousands of clean needles to drug users with the goal of reducing needle borne diseases, but faced significant pushback from some in the community.
As the state continues to grapple with the drug epidemic and its impact to public health, those running harm reduction programs in other West Virginia communities say the closure of the Charleston program, and the narrative that the needle exchange program was destroying the city, is having a negative impact on public perception of harm reduction efforts.
“Everyone understands that this drug epidemic is the biggest public health issue that we have dealt with,” said Terry Harlin, administrator of the Fayetteville harm reduction program. “I feel like what happened in Charleston hurt us a little bit.”
Harlin said when the Charleston program closed in , members of the community began questioning the necessity of the Fayette County program.
“We definitely started hearing people locally, ‘well it didn’t work in Charleston so why would you continue doing that here?’” she said. “Even though there’s lots of evidence and research out there that show that harm reduction does help to prevent the spread of disease and does help to get people the help that they need.”
A Shifting Narrative
The trickle effect to other programs like Fayetteville’s likely happened in the last six months the Kanwaha-Charleston program was open, when the narrative around the program shifted. Outgoing Charleston Mayor Danny Jones was especially outspoken critic of the program.
“Needles were everywhere and our property crimes went through the roof,” he said.
No study has been done quantifying whether the harm reduction program caused an increase in needle litter, making it hard to confirm the veracity of the claim. But we do know, according to data from the health department, that during the two years the program was open, more than 650,000 needles were distributed and only about 66 percent of them were returned.
West Virginia University public health researcher Robin Pollini said that doesn’t mean the unreturned needles ended up on the street. In West Virginia it is legal to dispose of sharps in the trash if you package them and label them in a certain way, she said.
“And so the Charleston program, just like many programs across the state, gives out puncture proof containers and information on how to dispose of those safely,” said Pollini. “And so we don’t have any idea how many of those ended up properly disposed of in household trash and how many didn’t.”
Dr. Susan Gardner, assistant dean of the University of Charleston School of Pharmacy, said she has seen little evidence of widespread needle litter. The school of pharmacy was one of the volunteer groups very involved in the Kanawha-Charleston Harm Reduction Program.
“There are times where I just took a walk on the East End looking — looking!,” she said. “[I say to myself] ‘ok, if it’s this bad surely I’ll see it.’ And the only time I’ve ever come across a needle in Charleston is doing a syringe cleanup.”
Us Versus Them
But without a study of Charleston’s needle litter, there’s also no way to prove that the 200,000 unreturned needles didn’t end up on the streets.
Members of the Charleston police department said they’ve observed much less needle litter since the program closed, but the department also has reams of photographs from first responders and community members of needles found in public spaces.
Comments on news articles and Facebook posts seem to paint a community drowning in needles.
On some level, needle litter itself, isn’t the issue.
“So part of the narrative that was built around the Kanawha program was this us and them of like ‘we’re the community and those people are drug users,’” said Pollini, from WVU. “Those people are part of our community they’re West Virginians right?”
In Wyoming County a Different Narrative
Wyoming County launched its needle exchange program in May. Executive Director Fred Cox said their program has been relatively well-received — he guesses because they had a small HIV outbreak prior to the program opening.
“A picture’s worth a thousand words I’d guess you’d say,” Cox said. “So, that picture was really clear to us here and I really do think that help changed some minds.”
He said if they hadn’t had the outbreak he doesn’t think they would have had to support to open the program as a prevention measure.
Some speculate that may be another reason Charleston’s program struggled in the end.
Outgoing Charleston mayor Jones said there were no reports of outbreaks of hepatitis C or the AIDS virus prior to the launch of the city’s harm reduction program.
“It’s not up to us to ruin a town over the fact that people have communicable diseases,” he said.
Rahul Gupta, formerly the head of the state’s public health department, said harm reduction is a multifaceted idea that encompasses not just needle exchange, but testing and family planning and treatment of diseases.
“And other issues that come across that are consequential in some ways like needle litter and other things there have to be plans in place to address those — what we can’t afford to do is ignore them,” he said.
There often are demands, Gupta said, to do things differently. But he believes there’s always a middle ground you can get to with negotiation. And you do that, he said, because “people’s lives are at stake.”
Part 4: Best Practices vs. Community Acceptance
Current best practices for harm reduction programs include a couple provisions: No retractable needles should be distributed, patients should get as many needles as possible regardless of how many they bring back, and barriers to accessing needles should be as low as possible. But sometimes those recommendations are at odds with community acceptance for the practices.

In late March, shortly after the Kanawha-Charleston Health Department closed its harm reduction program, Mayor Danny Jones wrote a letter to Rahul Gupta, then state commissioner for public health, asking that the West Virginia Bureau for Public Health audit the program.
“The review provided very specific recommendations that needed to be met in order to restart the program,” Gupta said.
These included improving data collection and analysis about exactly how many people were using the program and what services they were using; putting in place a plan to deal with needle litter; improving communication with community stakeholders and requiring that people pick up needles they need in person.
After the audit came out, the Kanawha-Charleston Health Department requested a review of the audit from seven harm reduction experts around the country, including Dr. Peter Davidson from the University of California San Diego. All seven letters were critical of the audit.
“I think the best way to describe it was that the people who wrote the audit had a very particular idea in mind about what a syringe distribution program should look like,” said Davidson.
In his letter Davidson wrote that “almost all of the recommendations in the audit represent severe, and in some cases unconscionable, barriers to effective, evidence-based, primary prevention of blood borne virus transmission.”
“You know one of the reasons syringe distribution programs exist in the way they exist at all is because is because the sort of traditional public health clinic model hasn’t served people who use drugs very well at all,” Davidson said. “And it hasn’t been very good at providing them with the basic tools they need in order to prevent the transmission of infectious disease and prevent overdose.”
Davidson said ideally, harm reduction programs have as low a barrier of entry as possible so the maximum amount of people will participate. And the recommendations made in the audit would raise the threshold of how easy it was to access resources, but he also says there’s room to adjust programs to fit the communities they serve.
“I wouldn’t expect a needle exchange in rural Appalachia to look the same as a needle exchange in San Francisco for example,” he said. “That would likely lead to a program that didn’t serve the population very well at all.”
And in Charleston, there were actually two harm reduction programs being held simultaneously: the one at the health department and a much smaller, clinic-based program operated by Health Right, the biggest free clinic in the state.
“Back in 2011 we noticed an increase in patients that were coming in with various stories, histories of being diabetic, they would pick up the needles for the program but not the insulin,” said executive director Angie Settle.
She said they began to suspect an increase in IV drug use among their patient population.
“So we kind of quietly started the program with the needle exchange it was mainly internal not something we broadcasted, but those patients that needed it knew of the service and as they came in we were screening every patient for IV drug use,” Settle said.
Because Health Right is a clinic working with a limited number of patients with whom they already have close relationships, they could run their program differently than the health department, which was trying to do a mass public health push, serving the whole city.
Health Right is also a one for one exchange — you bring a needle back, you get a fresh one — which for most harm reduction experts is not considered best practice. But since patients can come as many times a week as they want, Settle said it seemed to be the best choice for her program.
They also require every patient to meet with a counselor when they come in for needles. Basically, participation in Health Right’s program requires a lot more effort from patients, which means not everyone will use it, but Settle said that running a conservative program is preferable to not having a program available at all.
“You know the reality here is you’ve got a drug-using population that, in fact, is going to keep using drugs whether or not you have a syringe exchange program or not,” said Dr. Artis Hoven, an infectious disease specialist with the Kentucky Department of Health.
But without a program, she said, the community is just opening itself up to the easier spread of communicable diseases.
“There is something called the art and science, if you will, of risk or harm reduction,” said Hoven. “And for many of us we are still learning what that art is and what that science is. We’re trying to make it better and to make it something that is effective.”
But if Charleston were to consider harm reduction again, a lot of community healing, conversations, and compromise would likely have to occur. And the biggest barrier may be one of the most intangible ones — addressing stigma.
Part 5: A Community Divided
When the Kanawha-Charleston Health Department closed its harm reduction programs, one of the biggest criticisms of the program was that it led to an increase in crime, vagrancy and homelessness. Those claims are not without merit.

“I mean, that’s some of the stuff that people don’t really think about,” said Sgt. Matt Webb, who has been on the Charleston Police force for 20 years. During a ride-along, Webb was tracking a case of a man who was stealing vehicles and using them in other crimes. He pulled into an office parking lot where about eight cars were parked around a side-by-side ATV – effectively making it impossible to access the off-road utility vehicle.
“It’s the bigger picture of the drug issues. Guys out stealing somebody’s side-by-side … those people probably work hard every day to try to take care of their families and have things like that, and here he’s trying to support his drug habit and he goes and steals a side-by-side.”
During the 2018 mayoral election, crime and safety related to the drug epidemic became a political theme.
“One of the issues we have in our downtown area and is not just perception — it’s become reality unfortunately — is there is a belief that there is a public safety issue in downtown Charleston,” said mayoral candidate J.B. Akers during a fall debate between him and then-candidate Amy Goodwin televised by WCHS.
Akers was publicly critical of the syringe exchange component of the Charleston harm reduction program during his campaign. In the months leading up to the election, the program increasingly became a politically charged, divisive issue.
This fall, the City of Charleston completed a $100 million renovation on the Charleston Civic Center. The Civic Center overlooks the Elk River and abuts the Charleston mall. On other side? The Kanawha-Charleston Health Department.
“That health department shouldn’t be there,” said outgoing mayor Danny Jones.
The Charleston harm reduction program happened once a week. And as the program grew, that meant up to 400-some patients were coming through in a six-hour period for needle exchange as well as getting vaccinations, testing for diseases and accessing family planning services, among other services. This volume was a big deal for the downtown community.
“Having a program that was outside the city limits or at least within the city limits but in a less trafficked place by regular business people and people doing shopping in the city of Charleston would be an important thing to do as well,” said former city health officer Michael Brumage. Brumage said one of the lessons learned from the program was that they’d likely rethink the location.
Over the last couple of years, complaints of vagrancy and a rise in a criminal transient population have increased — a change Jones attributes to the harm reduction program and the geography of the state.
“It’s the confluence of the interstates,” he said.
Charleston is at the intersection of two major interstates — 64 running east to west and 77 running north to south, which Jones said made it easy for people outside of the city to come in and utilize resources meant for residents.
“I know it’s been a long time since I’ve started this profession, but when I first began this profession, I knew of two homeless people in town,” said Sgt. Webb. “And now, I mean, they’re all over the place.”
Sgt. Webb said that addiction and a bad economy go hand-in-hand.
“I’m pretty certain that the addiction aspect of what we’re dealing with has a lot to do with the economy,” he said. “You know, when you’re down on yourself you look for ways to make yourself feel better. I’m far from a doctor, but I’m sure a lot of people who are out here addicted to drugs had some kind of traumatic experience or they’re trying to fix something.”
A few months after the program closed, a Facebook group started, called “Charleston Has Had Enough!”, where members post photos of other people using drugs, stealing packages, panhandling, etc. Now, almost one of every 10 Charleston residents is a member.
None of the ten administrators or moderators returned requests for an interview, but in a Sept. 16 post, one of the founders wrote: “Word is going around that this group is all about shaming junkies. Anyone who believes that is an idiot. No. This is a group about shaming the so-called leadership that got us in the mess, namely the Kanawha County Health Dept. who convinced the city that free needles were a great idea.”
Danny Jones is a member.
“It was a really bad situation for our city. Needles were everywhere. Property crimes went through the roof. And now that it’s over, our property crimes have gone way down,” Jones said.
That’s a slightly misleading assertion. Larceny — meaning theft of personal property — has actually fallen considerably from 2014-2017, according to data obtained by West Virginia Public Broadcasting from the Charleston Police Department.
Burglary/breaking and entering spiked in 2016 (the first full year the program was in operation) but then fell to pre-program levels the second full year the program was in operation.
Breaking and entering into a car has risen continuously since 2014. And there was a massive spike in auto crimes in 2016 and no decline during the program’s second year of operation. But data like this does not prove why some crime went up after the harm reduction program opened and some went down. And speculations only seem to divide community.
In an off-the-record conversation, a member of the Charleston Fire Department said the closure of the Charleston program had set the city back 10 years in terms of acceptance of harm reduction. How to move forward is a subject incoming mayor Amy Goodwin addressed in the October debate televised by WCHS.
“Leaders lead,” she said. “Leaders don’t take the blame or cast the blame on someone else. They look at what they’ve done wrong and they say, ‘let’s improve it.’ They look at something that may be a problem in the city and they work with everyone; they bring everyone to the table. They don’t villainize; they don’t marginalize folks.”
At this point, bringing everyone to the table is going to take a lot of work, but it’s not impossible.
“I would be interested in being on some kind of board where they hold discussions about trying to find answers to these questions,” Sgt. Matt Webb said. He said it’s really challenging working with a population struggling with addiction.
“It’s frustrating,” he said. “If we go to somebody’s house and they’re having a heart attack, we send them to a doctor and the doctor can hopefully fix their heart. They give them a heart cath, they give them open heart surgery, they’ll do bypass – whatever. When it comes to somebody who is addicted to opioids – a lot of times, I know it’s not true, but they give off the impression that they don’t want help but it’s because the addiction is so great they feel like they don’t want help.”
And if someone does want help, he said, it doesn’t get much easier.
“Are there beds available in rehab places? How are they going to pay for it? Those are sometimes hard answers to get.”
But whether a board is created to discuss these issues like Webb mentioned — or even if enough people are willing to sit down and really listen to one another to address the still present public health risk of needle borne diseases — remains to be seen.
This series was originally published by West Virginia Public Broadcasting. Read them individually: Part 1, Part 2, Part 3, Part 4 and Part 5.



